A sick health system
The suspension of three doctors following the death of Chimamanda Ngozi Adichie’s son has renewed scrutiny of a health-care system plagued by impunity, underfunding, and a mass exodus of medical professionals.
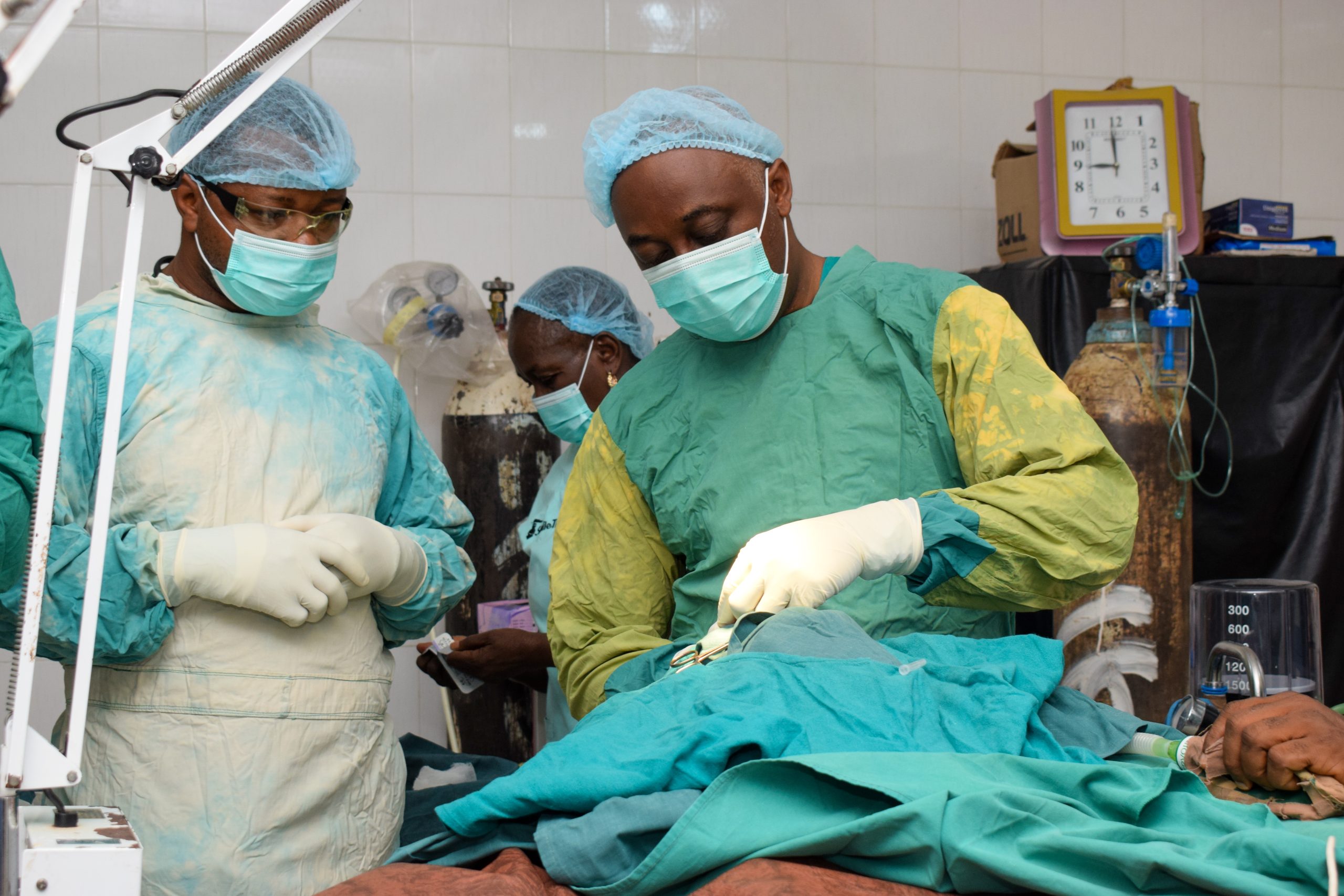
A hospital in Abuja, Nigeria. Image credit Oni Abimbola via Shutterstock © 2021.
The Medical and Dental Council of Nigeria (MDCN) has suspended three medical doctors, including a medical director, in connection with the death of Chimamanda Ngozi Adichie’s 21-month-old son.
In January, the acclaimed Nigerian author accused Euracare, a private hospital in Lagos, of negligence after her child was sedated for an MRI scan and a central line procedure in preparation for his imminent evacuation from Nigeria to the United States, where a medical team was on standby.
In a leaked message Adichie shared with friends and family, she alleged the anesthesiologist broke several medical protocols, including administering an overdose of propofol and denying her child oxygen. She also claimed the same anesthesiologist had been involved in two other deaths and questioned why he was still allowed to practice.
For its part, Euracare has denied any wrongdoing; a disciplinary tribunal and an inquest into the child’s death are pending.
Tales of gross medical negligence and incompetence abound in Nigeria. Hospitals are notorious for denying care to patients with gunshot wounds without a police report absolving them of wrongdoing. It’s also not uncommon to find doctors, especially those working in public hospitals, displaying crude bedside manners or little concern for patients’ well-being. Consultations are treated like nuisances, with doctors responding dismissively to patients, as though afraid their inquiries would expose their lack of knowledge.
“Their attitude is so hostile to patients and relatives, yet we provide everything right down to gloves,” said Timi,* whose relative was admitted a few years ago at a government-owned hospital, where medication and medical accoutrements are often provided by patients and caregivers. “All that is asked of them is their humanity and expertise.”
The nonchalance and disdain extends beyond the consultation room into hospital wards and theaters, where it sometimes mixes with a heavy dose of misogyny. It’s no secret that pregnant women face abuse and neglect from doctors and nurses while giving birth. Some female patients have been sexually assaulted or asked intrusive, medically irrelevant questions during their gynecological exam.
A caregiver, Edet,* recalled how a male doctor had approached her mother’s bedside and without a word to either of them started lifting her dress. She stopped him immediately.
“He didn’t say, ‘Excuse me,’” Edet said of the ill-mannered physician. “[He] just came and started pulling it up.”
Eventually, she allowed the doctor to palpate her mother’s stomach. But even then, he didn’t communicate his findings until she asked.
Many have also criticized the general apathy and lack of professionalism among medical staff in Nigeria. During their stint as a caregiver, Timi said they witnessed a doctor respond to a late-night emergency without any sense of urgency.
“He strolled out with red eyes and his boxers peeking out of his scrubs, looking like a motor-park tout,” they said, adding that the same doctor had spoken rudely to a patient calling for help on a different night.
“He turned around and said to the patient, ‘Even the security man is sleeping at this time, let alone me.’ But if someone is calling your attention, then it means there’s something wrong.”
With little to no fear of censure from their indulgent employers and the somnolent MDCN that regulates medical practitioners, doctors in Nigeria can and do operate with impunity. It doesn’t help that the masses are too meek, frazzled, impoverished, ignorant, or demoralized to file lawsuits or lodge formal complaints against medical malpractice. And even if one wishes to take such actions, hospitals have made it near impossible as some deliberately allow their staff work without name tags to prevent disgruntled patients from publicly naming and shaming unscrupulous doctors and nurses.
Apart from the lax regulatory environment, the medical field suffers from a combination of structural issues that further hampers quality health-care delivery.
For one, Nigeria’s health-care allocation currently stands at a meagre 4.2 percent of the total budget, painfully inadequate for a population of 220 million. Due in part to the government’s decades-long lack of investment in health care, thousands of frustrated, underpaid, and overworked medical practitioners continue to migrate to Western countries every year, with the result that Nigeria currently has just 55,000 doctors, far less than the World Health Organisation’s recommended ratio of one to 600 patients.
Then there’s the perennial issue of corruption, which saw a former first lady lament the lack of syringes and medication during her visit to the State House Clinic in 2017 despite the billions of naira allocated to it.
Of course, none of these statistics matter to the political elite, not when high-ranking government officials—including the president—travel abroad for medical treatment. As such, there’s little incentive to fund public hospitals or even address the poor working conditions plaguing the medical field.
Yet one must realize that underinvesting in health care isn’t a new phenomenon. During colonial rule, few hospitals were built to cater to the local population, a problem that worsened under the torturous structural adjustment programs (SAP) of the 1980s. Conceived by the International Monetary Fund and World Bank, the so-called economic fix demanded African countries slash funds for public goods (education, roads, salaries, sanitation, and yes, health care) and sell off government assets to private investors as a precondition for much-needed loans. Health-care delivery became a marketable commodity, with private hospitals encroaching on the services public ones were struggling to provide, while the gap between the impoverished masses and policy makers widened.
In a recent op-ed for the British Guardian, Botswana President Duma Gideon Boko touched on this exact problem, explaining why his government was nationalizing the country’s largest private hospital.
“Greater reliance on private provision fragments care, raises costs and diverts scarce health budgets into profit margins. [ . . . ] But when shortages hit, it is the government that people turn to. Democratic responsibility cannot be subcontracted.”
Although present-day consensus admits SAP sapped African economies by insisting governments earmark a large percentage of their national budget for interest repayment, resource theft by the Global North continues apace with little consideration for the knock-on effects. For instance, Britain, having defunded its much-beloved National Health Service (NHS), now poaches doctors and nurses from Africa to fill in slots vacated by its own medical staff who have left the UK for Australia for better pay and working conditions. (Britain’s austerity measures have resulted in crumbling hospitals, exploited doctors, and disgruntled patients—including those with cancer—waiting at least a year for a doctor’s appointment.)
In an ironic twist, the WHO cautioned the British government about actively recruiting medical staff from Nigeria, Ghana, and Sudan, countries already suffering from a dangerously low doctor-patient ratio. Also, the fact that many Nigerian-trained doctors attend public universities subsidized by their government adds another seedy element to Britain’s rapacious behavior.
Treating Nigeria’s hazardous health-care system will require more than sacking one, two, or three inept doctors, or as the current trend predicates, setting up another “state-of-the-art” for-profit hospital in a major city. Rather, the cure resides in enforcing patient-safety protocols, insisting on professionalism among doctors, and holding accountable hospitals that flout medical ethics. More importantly, if health services are to meaningfully improve, the government must increase the amount allocated to health care.