‘We are workers, not heroes’
African health workers ask for decent work and a strong, public health care system — not applause.

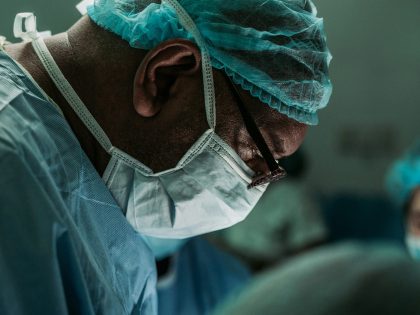
Healthworker in Liberia. Image via US AID on Flickr.
Writing in the UK Guardian in March 2020, the Liberian nurse and union leader George Poe Williams, feared that, like during the Ebola crisis, COVID-19 will lead to deaths that could be avoided unless we abandon austerity policies and build a strong public health system. The correct policy response would also require jobs in the public sector, and that health workers get proper working conditions. “We health workers are not heroes,” Poe Williams wrote. “We should not become martyrs at work. We are professionals. We need personal protective equipment so that we can maintain health while saving lives. We need adequate staffing and well-equipped health systems. We need strong public funding for our sector.”
During the Ebola crisis in 2014, health workers in Liberia made concrete choices about life and death: they had to choose between which patients to try to save and those who were likely to die; they had to choose between going to work risking infection (and death) or not going to work. At the time of Ebola, the National Health Workers Union of Liberia (NAHWUL), of whom Poe Williams is a member, fought for better resources and personal protective equipment (PPE). Today, Poe reflects that a lack of response from the authorities contributed to the fact that eight percent of Liberian health workers died.
The health sector in many countries was in crisis even before the COVID-19 crisis. Underfunding and understaffing of the public health system means that many in the world do not have access to health. The logical consequence should be to build a public health system, possibly with international development assistance.
Since COVID-19 went global, we have seen strikes from health workers around the world, which may seem unusual, considering medical staff are seen as essential workers and rarely go on strike.
Admittedly, some strike threats have been about pay. While “ghost workers” are reported on public payrolls in Kenya, i.e. names often of friends or the family of politicians, Nigerian doctors and Liberian nurses dropped off payrolls in 2020 and 2018 respectively. It is not uncommon for public employees in African countries not to be paid wages for work performed. Even when the Ebola virus came to Liberia in 2014, NAWHUL was in such a strike—or a slow-action—for the payment of non-paid wages, but it was interrupted to return to work to counter the Ebola virus.
Both the Liberians in 2014 and the Nigerians in 2020 combined payroll requirements with protective equipment requirements. In most cases this is what’s needed: training and protection requirements. This is also the main requirement of professional associations across Africa: that workers have PPE. It’s about fear of death and professionalism, not greed.
While health care professionals around the world are defined as essential and exempt from coronavirus measures, they also have exceptions to labor rights. The right to strike is restricted for reasons of public health, based on international labor conventions. But both the World Health Organization (WHO) and the Global Association of Public Employees, PSI (Public Service International) point out that in many countries, the limits on rights limitation are far beyond acceptable. This is just one of the reasons why healthcare workers often have low wages, such as in the UK and the United States; income for workers is defined as income to be able to meet workers’ family’s basic needs). In 2014, the salaries of health workers in Liberia were described as “ridiculous” by a Norwegian TV anchor. Across the world, the health sector, with a large number of migrants and a majority of women, is characterized by heavy work pressure and part-time and short-term contracts, while also suffering from under-staffing and unsustainable shift schemes.
In 2016, the WHO recommended creating at least 40 million new jobs in health and social care, especially in poor countries, to reach the sustainability goals by 2030. This year came a new report from WHO that the world needs 9 million new nurses. In Nigeria alone, 500,000 to 600,000 nurses are needed. At the same time, the African Union, the United Nations Development Program and the International Labor Organization fear that the COVID-19 crisis could lead to the loss of 20 million jobs in Africa.
African heads of state are now confronted with a health care system they have neglected for years. African elites have often traveled abroad for treatment. Zimbabwe’s Robert Mugabe died at a hospital in Singapore. Nigerian President Mohammadu Buhari has traveled to the UK several times (one time for almost two months), while one of his predecessors, Umaru Musa Yar’Adua, preferred the hospitals in Saudi Arabia (he eventually died there). African heads of state are to blame, but we must also remember a long history of international demands. Underfunding of the health sector is also linked to borrowing requirements for public savings from the International Monetary Fund and the World Bank. But today even the IMF recommends increased investment in the Nigerian health care system.
Social security is also an integral part of the decent working life agenda in Sustainability Goal 8 of the United Nations, which unfortunately is often reduced to mean just job creation (in the private sector). Trade union PSI recalls that although the right to health is enshrined in no less than 150 countries’ constitution, privatization has meant that access to health is unfairly distributed and dependent on class. Without private health insurance, which is often linked to work, the right for many becomes a theoretical exercise. In Africa, many of the 70 percent of the informal sector’s workforce have weak or poor access to health. During the coronavirus crisis we are reminded that this is not only unfair, but dangerous for the more privileged of us.
It is not only the health workers at PSI who insist that public health is more resilient, strong and fair. A partially privatized health care system is fragmented and unable to effectively coordinate infection control. To address the coronavirus crisis, both Ireland and Spain have nationalized health enterprises. In Norwegian aid, health and education are two of the most important development goals. Both should be linked to job creation and workers’ rights.